Surgery for thyroid cancer
Surgery is a medical procedure to examine, remove or repair tissue. Surgery, as a treatment for cancer, means removing the tumour or cancerous tissue from your body.
Most people with thyroid cancer have surgery. The type of surgery you have depends mainly on the type, stage and risk group of the cancer. When planning surgery, your healthcare team will also consider other factors, such as the stage, your age and your overall health.
Surgery may be the only treatment you have, or it may be used along with other cancer treatments. You may have surgery to:
- completely remove the tumour
- remove as much of the tumour as possible (called debulking)
- remove lymph nodes
- relieve pain or other symptoms (called palliative surgery)
Surgery for thyroid cancer may be done using different techniques. Standard surgery involves a larger cut (incision) near the middle of the neck. Endoscopic surgery involves a smaller incision near the middle of the neck, where an endoscope is inserted and a video monitor is used to guide the surgery.
The following types of surgery are used to treat thyroid cancer.
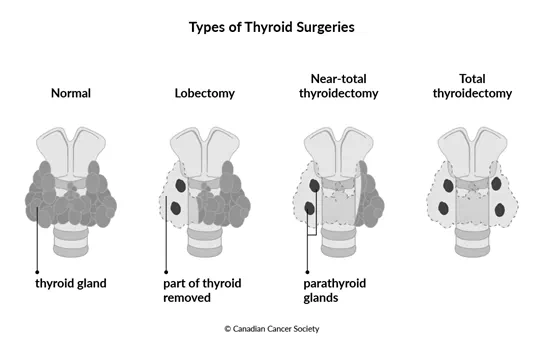
Lobectomy
A lobectomy is surgery to remove the one side, or lobe, of the thyroid that contains cancer. A lobectomy is also called a partial thyroidectomy, or hemi-thyroidectomy.
Sometimes cells collected from a lump in the thyroid during a fine needle aspiration (FNA) biopsy look a lot like normal thyroid cells (they are well-differentiated). Doctors can't tell if the lump is a benign (non-cancerous) thyroid nodule or a cancerous tumour. When this happens, doctors do a lobectomy to help make a diagnosis.
A lobectomy may be used to treat low-risk papillary thyroid cancer. It can be used if the tumour is only in the thyroid, has not grown through the thyroid or spread to other parts of the body and is 4 cm or smaller.
Near-total thyroidectomy
A near-total, or subtotal, thyroidectomy is surgery to remove most of the thyroid gland. Doctors will remove as much thyroid tissue as they can without damaging any other structures in the neck. It is used to avoid problems that can happen when all of the thyroid is removed.
Total thyroidectomy
A total thyroidectomy is surgery to remove the entire thyroid. It is the most common type of surgery done for thyroid cancer.
A total thyroidectomy can be done for papillary or follicular (including Hurthle cell) thyroid cancer in any risk group, especially if the doctor plans to use radioactive iodine (RAI) therapy after surgery. It is also the first treatment for medullary thyroid cancers. A total thyroidectomy is rarely used to treat anaplastic thyroid cancer.
Neck dissection
A neck dissection is surgery to remove several lymph nodes from the neck. The surgeon may also remove other tissues around the thyroid. It is often done at the same time as a thyroidectomy.
A neck dissection is usually done when:
- the doctor thinks there is cancer in the lymph nodes in the neck based on the results of an ultrasound or a CT scan
- a biopsy shows there is thyroid cancer in the lymph nodes
- the cancer has a high risk of spreading to the lymph nodes
The type of neck dissection done depends on the size of the tumour and which lymph nodes in the neck the doctors think have cancer in them. The most common type of neck dissection for thyroid cancer is a central neck dissection. This surgery removes lymph nodes from the front of the neck near the thyroid. Doctors may also do a functional neck dissection or modified radical neck dissection if they need to remove more lymph nodes from the sides of the neck.
Find out more about neck dissection.
Surgery for advanced thyroid cancer
The following types of surgery are used to remove as much cancer as possible and relieve symptoms of advanced thyroid cancer.
En bloc resection may be done to remove the tumour, surrounding tissues, lymph nodes and structures in the neck as one piece (en bloc). This surgery may be used to treat anaplastic thyroid cancer that has spread outside of the thyroid to tissues and structures in the neck.
Surgery for metastasis may be used to remove thyroid cancer that has spread, or metastasized, to distant organs such as the lungs, brain or liver.
Palliative surgery may be done if a large tumour causes symptoms or blocks an airway or the esophagus. The surgeon will remove all of the cancer or as much of it as possible (called debulking).
Tracheostomy is a surgical procedure to create an opening (called a stoma) in the trachea (windpipe) through the neck so air can reach the lungs. It is needed when a tumour presses on or blocks the trachea and makes it difficult to breathe. Find out more about living with a tracheostomy.
Side effects of surgery
Side effects of surgery will depend mainly on the type of surgery and your overall health. Tell your healthcare team if you have side effects that you think are from surgery. The sooner you tell them of any problems, the sooner they can suggest ways to help you deal with them.
Lobectomy, total thyroidectomy and neck dissection may cause these side effects:
- hoarseness or other voice changes
-
numbness and tingling feelings (often in the face) and muscle spasms caused
by low levels of calcium in the blood (called hypocalcemia) and damage to
the
parathyroid gland - wound infection
- swallowing problems
- breathing problems
A neck dissection may also cause weakness in the neck and shoulder.
Find out more about surgery
Find out more about surgery and side effects of surgery. To make the decisions that are right for you, ask your healthcare team questions about surgery.
Your trusted source for accurate cancer information
With support from readers like you, we can continue to provide the highest quality cancer information for over 100 types of cancer.
We’re here to ensure easy access to accurate cancer information for you and the millions of people who visit this website every year. But we can’t do it alone.
Every donation helps fund reliable cancer information, compassionate support services and the most promising research. Please give today because every contribution counts. Thank you.
