Tracheostomy
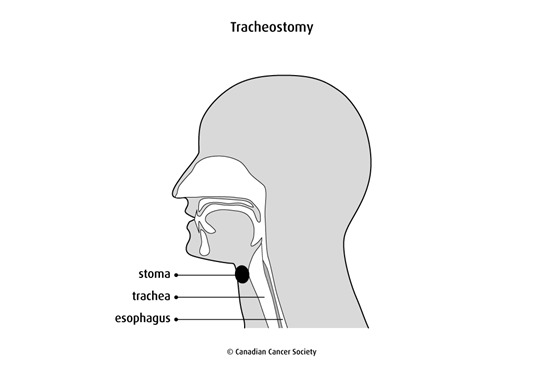
A tracheostomy is a surgical procedure to create an opening (stoma) through the neck into the trachea (windpipe). It helps a person breathe. A tube placed through the stoma creates a new path for air to reach the lungs.
A tracheostomy is done if the upper airway is narrowed or blocked. It can also be done as part of a laryngectomy, which is surgery to remove the larynx (voice box).
- If you have a partial laryngectomy, the stoma is usually temporary. After you’ve recovered, your doctor removes the tube, and the stoma heals closed. Your voice and breathing may be different. They do not always return to the way they were before surgery. Your voice may be different after the tube is removed, especially if the vocal cord is removed.
- If you have a total laryngectomy, the stoma is permanent. You will breathe through the stoma and learn to speak in a new way.
Living with a tracheostomy requires some changes to your life. Most people adjust well after they have had some time to get used to the change. Your healthcare team will teach you about living with and caring for your tracheostomy.
Stoma tubes
Different types of tubes are placed in the stoma depending on whether your tracheostomy is temporary or permanent. A tracheostomy tube is used for a temporary stoma and a laryngectomy tube is used for a permanent stoma. Most tubes are made of disposable plastic and can be used for a few weeks or months.
Protecting the stoma
When you breathe, the air is normally cleaned, warmed and moistened as it passes through the nose and mouth. With a stoma, the air goes directly into the trachea without being moistened. The dry air can thicken mucus that is in the lungs and trachea, which can make it hard to breathe. Water, dust, smoke and other particles in the air can enter the stoma, making you cough or choke. If the stoma isn’t covered, mucus is coughed out of the stoma directly into the air.
You can try the following to protect the stoma and avoid these problems.
- Stay well hydrated to help keep the mucus thin.
- Spray a sterile salt solution into the stoma, as instructed by your doctor or stoma nurse.
- Use humidifiers, especially during the winter when indoor air can become dry from central heating.
- Wear a cover over the stoma.
Routine care of the stoma
Daily care is needed to keep the stoma clean. Before you leave the hospital, your healthcare team will teach you how often stoma care should be done. They will also teach you how to:
- remove, clean and replace the tube
- care for the skin around the stoma
- use a suction tube to remove mucus, if necessary
Bathing and showering
You can still bathe and shower as you did before, as long as the stoma is covered so that water does not get into the opening. You can buy special shower shields for this purpose.
If your neck is numb after surgery and you need to shave, avoid cutting yourself by using an electric razor.
Changes to smell and taste
After surgery, your ability to smell will change because air no longer passes through your nose. For a few weeks after surgery, your nose may be sore and runny as its tissues adjust to the lack of air flow. This is normal and will improve over time.
A method called “polite yawning” may help improve smell. It is basically yawning with the mouth closed. Air is drawn into the nose by keeping the mouth closed and covering the stoma. The air passing through the nose allows you to smell.
Taste will also be affected because it is closely tied to smell. You may want to talk with a dietitian about foods that have a stronger flavour. Ask for tips on how to prepare food so that it tastes better. You may want to try marinating foods before cooking or adding more spices while cooking.
Swimming and other water sports
You will need special equipment to go swimming with a stoma. Your healthcare team will be able to give you more information about equipment that is available. Other water sports, such as diving or water-skiing, are not recommended because of the danger of water entering the stoma.
Body image
Having a tracheostomy may affect how you feel about your body and change your body image. It is common to have concerns, fears and anxiety about your appearance and changes to your body function. Some people even have trouble looking at their stoma at first. Talking about these feelings and realizing that it will take time to adjust can help you become more comfortable.
Work
After recovering from surgery, most people with stomas can return to work with no problems. An exception may be for people who have jobs that involve heavy lifting. Heavy lifting requires a person to hold their breath, and people with a stoma can’t do this. Some people may need to adjust their work situation.
Emergency identification
If you have a tracheostomy, you should always carry identification that explains your medical condition. This can be a wallet card or jewellery that will alert emergency workers to your special breathing needs.
Your trusted source for accurate cancer information
With support from readers like you, we can continue to provide the highest quality cancer information for over 100 types of cancer.
We’re here to ensure easy access to accurate cancer information for you and the millions of people who visit this website every year. But we can’t do it alone.
Every donation helps fund reliable cancer information, compassionate support services and the most promising research. Please give today because every contribution counts. Thank you.
