Thyroid problems
Thyroid problems can develop with certain types of cancer and after some cancer treatments. People who are treated for Hodgkin lymphoma and brain and spinal cord tumours have a higher risk for thyroid problems. People treated for cancer during childhood have an even greater risk. Thyroid problems can happen in the first few months or years after diagnosis and treatment.
How the thyroid works
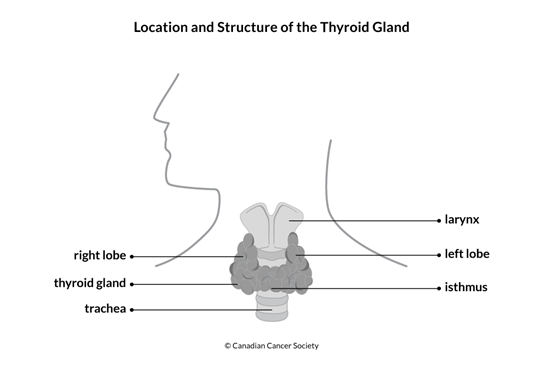
The thyroid is a gland in the lower part of the neck. It sits in front of the
trachea (windpipe) and below the larynx (voice box). The thyroid is part of the
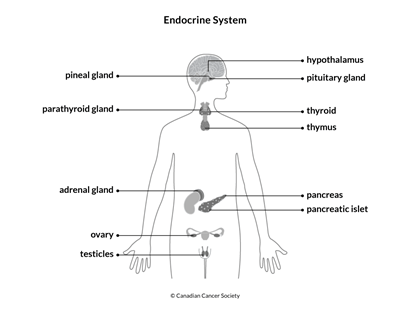
The thyroid makes thyroxine and triiodothyronine. These hormones are involved in growth and mental development. They also help regulate metabolism, which is the chemical processes in the body that create and use energy.
The thyroid is controlled by the pituitary gland. The pituitary gland makes thyroid-stimulating hormone (TSH). It releases TSH in response to thyroxine and triiodothyronine levels in the blood. TSH signals the thyroid to make more hormones.
Causes
The following cancer treatments can cause thyroid problems.
Radiation therapy
Having radiation therapy to or near the thyroid or pituitary gland can increase the risk for thyroid problems. The risk is greater for people treated with higher doses of radiation and at a younger age. Women often have a higher risk than men. People treated with radiation to the head and neck are 2 times more likely to develop thyroid problems than other cancer survivors.
The following can also increase the risk for thyroid problems:
- radiation therapy to the head, neck, upper chest or spine
- total body irradiation (TBI) before a stem cell transplant
- radioiodine (I-131) therapy
- high doses of metaiodobenzylguanidine (MIBG), which is sometimes used to treat neuroblastoma
Drug therapies
The following drug therapies can increase the risk for thyroid problems:
-
alkylating chemotherapy drugs, such as cyclophosphamide (Procytox) or busulfan
-
tyrosine kinase inhibitors, such as imatinib (Gleevec) or dasatinib (Sprycel)
-
the monoclonal antibody alemtuzumab (Lemtrada)
-
immune checkpoint inhibitors, such as ipilimumab (Yervoy) or bevacizumab (Avastin)
Surgery
Surgery to remove the thyroid causes thyroid problems.
Types of thyroid problems
Thyroid problems that can develop after cancer treatment include the following.
Growths on the thyroid may be non-cancerous (benign) or cancerous (malignant). Both usually start as slow-growing, painless lumps in the neck.
Hyperthyroidism is when the thyroid makes too much thyroid hormone.
Hypothyroidism is when the thyroid doesn't make enough thyroid hormones. There are different types of hypothyroidism. Primary hypothyroidism is caused by damage to the thyroid or surgery to remove the thyroid. Central hypothyroidism is caused by damage to the hypothalamus or pituitary gland in the brain. Compensated hypothyroidism happens when the pituitary gland has to constantly tell the thyroid to make hormones to keep normal hormone levels in the blood.
Symptoms
Symptoms of thyroid problems can vary depending on the type of problem.
Growths on the thyroid may cause:
-
hyperthyroidism
- pain in the neck, jaw or ear
- difficulty swallowing
- shortness of breath
Hyperthyroidism may cause:
-
jitteriness, nervousness or anxiety
- problems concentrating
- moodiness
- feeling tired
- muscle weakness
- shaky hands, or tremors
- fast or irregular heartbeat
- increased sweating
- feeling hot all of the time
- diarrhea
- weight loss
- irregular menstrual periods
- bulging, or protruding, eyes
- neck tenderness and swelling
- low exercise tolerance, which is fatigue or shortness of breath during mild exercise
- trouble sleeping
- increased appetite
- goitre, which is an enlarged thyroid
- thinning hair or hair loss
Hypothyroidism may cause:
-
hoarse voice
- feeling tired
- problems concentrating
- feeling sad or depressed
- mood changes
- constipation
- weakness
- feeling cold all the time
- puffiness of the face (especially around the eyes) and hands
- weight gain
- dry skin
- brittle hair and fingernails
- muscle and joint aches
- growing more slowly than normal
- puberty starting at an older age
- slow heart rate
- low blood pressure
- high cholesterol level
- low exercise tolerance, which is fatigue or shortness of breath during mild exercise
If symptoms get worse or don't go away, report them to your doctor or healthcare team without waiting for your next scheduled appointment.
Diagnosis
Thyroid problems are usually diagnosed by:
- physical exam to check growth and development
- blood tests to check thyroid-stimulating hormone (TSH) and free thyroxine (T4) levels
- an ultrasound to check the size of the thyroid and if there are nodules (lumps) on it
Find out more about these tests and procedures.
Managing thyroid problems
Different treatments are used to manage different thyroid problems.
Growths on the thyroid are tested using an ultrasound and a biopsy to check if they are cancerous. Surgery may be done to remove the growths.
Hyperthyroidism may be treated in several ways, including medicine, surgery to remove the thyroid or thyroid ablation. Thyroid ablation is a treatment that destroys the hormone-producing cells with a radioactive substance, such as radioiodine (I-131).
Hypothyroidism can be treated by taking medicine each day. Most people have to take medicine for the rest of their lives. In some cases, it may be stopped if the thyroid begins to work normally.
Follow-up
All people who are treated for cancer need regular follow-up. The healthcare team will develop a follow-up plan based on the type of cancer, how it was treated and your needs.
Make sure you tell your doctor all the treatments you received. If you received radiation therapy to the head or neck, you should have a physical exam each year. Follow-up tests may include blood tests to check thyroid-stimulating hormone (TSH) and free thyroxine (T4) levels.
Your trusted source for accurate cancer information
With support from readers like you, we can continue to provide the highest quality cancer information for over 100 types of cancer.
We’re here to ensure easy access to accurate cancer information for you and the millions of people who visit this website every year. But we can’t do it alone.
Every donation helps fund reliable cancer information, compassionate support services and the most promising research. Please give today because every contribution counts. Thank you.
